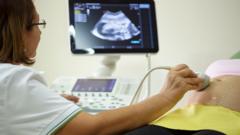
The gel is always cold. It is a small, sharp shock against the skin, a clinical greeting that usually precedes the most significant moments of a person’s life. In a dim room, a sonographer moves a plastic transducer across a patient’s abdomen, looking for the flickering pulse of a heartbeat or the jagged shadow of a tumor. But lately, the rooms are staying dark. The machines are silent.
Sarah—a hypothetical composite of the thousands currently caught in the healthcare backlog—doesn't know about the national shortage of sonographers. She doesn't know that over 10% of ultrasound posts in the public health sector are vacant, or that the equipment is aging faster than it can be replaced. She only knows that she found a lump three weeks ago. She knows the GP marked her referral as urgent. And she knows that when she called the hospital, the voice on the other end sounded tired, almost defeated, as they told her the next available slot was two months away.
Two months is an eternity when you are staring at the ceiling at 3:00 AM, wondering if the cells inside you are dividing.
The Invisible Bottleneck
We often think of medical crises in terms of flashing lights and sirens. We imagine the drama of the operating theater or the high-stakes rush of the emergency room. But the real crisis in modern diagnostics is quieter. It is the sound of a telephone ringing in an empty office. It is the sight of a "Position Vacant" notice that has been pinned to a staff room board for a year.
Ultrasound is the workhorse of the medical world. It is portable, radiation-free, and relatively inexpensive compared to the multi-million-dollar behemoths of MRI and CT scans. Because of its versatility, it is used for almost everything: monitoring the development of a fetus, checking for gallstones, guiding needles for biopsies, and screening for deep vein thrombosis. It is the primary gateway to treatment. If that gate is locked, the entire hospital system grinds to a halt.
When sonographers warn that delays are putting lives at risk, they aren't being hyperbolic. They are describing a mathematical certainty. In the case of suspected cancer, the difference between Stage 1 and Stage 4 is often measured in weeks. When a diagnostic test is pushed back by sixty days, the "wait and see" approach becomes a "wait and suffer" reality.
The Human Cost of Efficiency
Consider the pressure on the person holding the probe. A sonographer’s job is a strange blend of high-level physics, anatomy, and emotional labor. They are often the first person to see that a pregnancy is no longer viable or that a mass has the irregular, jagged edges of malignancy. They must maintain a neutral, professional mask while their eyes communicate a truth the patient isn't yet ready to hear.
Now, imagine doing that sixty times a day.
Professional burnout in the imaging sector has reached a tipping point. The workforce is aging out, and the pipeline of new recruits is leaking. Training a sonographer is not a quick process; it requires years of specialized postgraduate study. You cannot simply pull a nurse or a general practitioner off the ward and ask them to interpret the grainy, shifting shadows of an internal organ. It is a craft.
But the craft is being crushed by the quota. To clear the post-pandemic backlog, many departments have increased their "throughput." This is a sterile, corporate word for squeezing more people into less time. When a twenty-minute scan is compressed into twelve, the margin for error grows. The risk of a missed diagnosis increases. The sonographer’s wrist and shoulder—already prone to repetitive strain injuries—begin to fail.
The system is cannibalizing its own experts to keep the numbers moving.
A Shadow on the Screen
Let’s return to the stakes for the patient. In maternal health, an ultrasound is meant to be a moment of connection. It’s the "big reveal." But for women experiencing pain or bleeding in early pregnancy, the scan is a lifeline of information. When those scans are delayed, women are forced to sit in a state of biological limbo. They are physically pregnant, but emotionally suspended, unable to grieve or move forward because the diagnostic proof is stuck in a digital queue.
Then there are the vascular patients. A suspected blood clot in the leg is a ticking clock. If it stays in the leg, it is a problem. If it breaks loose and travels to the lungs, it is a catastrophe. In a functional system, an ultrasound happens within hours. In a strained system, it happens within days.
The risk isn't just that people are dying; it’s that the quality of the life they have left is being degraded by preventable anxiety. Uncertainty is a form of physical pain. It raises cortisol, ruins sleep, and fractures families. We are currently asking citizens to pay a "stress tax" because we failed to invest in the humans who operate the machines.
The Breaking Point
The math of the crisis is simple, even if the solution is not. We have more people who need scans than we have people to perform them. Population growth, an aging demographic, and the rising prevalence of chronic diseases have created a surge in demand that the current workforce cannot meet.
Some suggest that Artificial Intelligence will be the savior, that algorithms will eventually be able to interpret these images with the click of a button. But an algorithm cannot feel the resistance of a patient’s muscle or adjust the angle of a probe to see around a layer of scar tissue. An algorithm cannot hold a hand when the screen goes still.
The solution requires a fundamental shift in how we value diagnostic labor. It means funded training spots, better retention strategies, and a realization that a hospital is only as good as its ability to see what is happening inside its patients.
Beyond the Statistics
Data points on a spreadsheet don't bleed. They don't have children or mortgages or favorite songs. But every "delayed appointment" in the national database represents a person like Sarah, sitting in a plastic chair in a waiting room, staring at a clock that seems to be moving backward.
The tragedy of the current ultrasound shortage is that the technology is right there. The machines are sitting in the rooms. The electricity is humming. The gel is on the counter. We have the tools to save lives, to provide clarity, and to offer peace of mind. We just lack the hands to pick up the tools.
As the sun sets over a suburban hospital, a light stays on in the imaging department. A lone sonographer is finishing her fourteenth hour of work. She is tired. Her back aches. She looks at the list of names for tomorrow and knows she won't get through them all. She thinks of the faces she saw today—the relief, the terror, the numb silence.
She picks up the transducer and cleans it for the final time tonight. Tomorrow, the waiting starts again. Tomorrow, more people will find themselves caught in the gap between a symptom and a certainty. We are living in a silent era, defined not by what we can see, but by all the things we are choosing to ignore.
The gel is cold. The room is dim. The screen is waiting for a pulse.